What is Rotator Cuff Tendonitis?
Firstly, Tendonitis:
In truth, the word tendonitis should probably not exist. Research has shown that it is very uncommon for tendons to be inflamed. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3312643/
Rather,than tendons becoming inflamed, their structure changes and alters its ability to function, causing pain. To this end, it is more correctly called tendonosis or tendonopathy. This leads to many a discussion about whether steroid injections targeting the ‘inflammation’ is appropriate or even if ibuprofen should be the painkiller of choice. http://www.bmj.com/content/324/7338/626.full
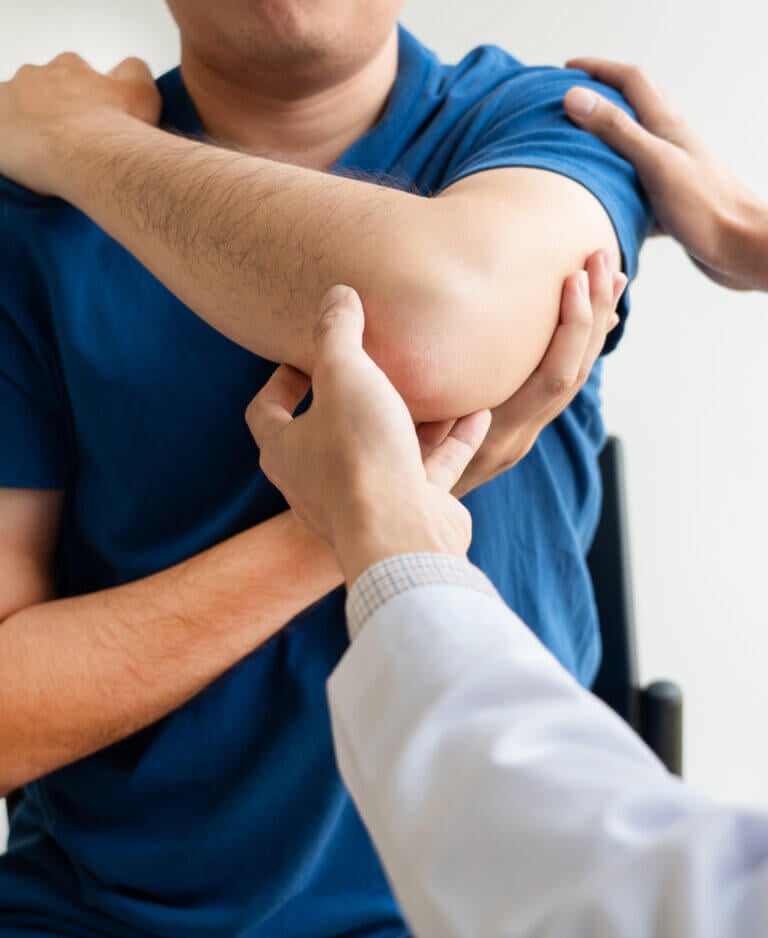
Rotator cuff: The rotator cuff is a group of 4 muscles with a common inserion area on the humerus. Without going into the anatomy, it is usually one of them, the supraspinatus, which causes the condition we are addressing.
The supraspinatus passes underneath an arch called the acromium, which forms the acromio-clavicular joint. The are also bursae (which can be inflamed) under this joint and muscle. When the supraspinatus becomes irritated under this structure, we can get a tendonopathy. The muscle/tendon essentially doesn’t function well under this tight space and its parallel fibres become higgledy piggledy. This makes movements like putting a coat on, bra strap, seat belt, pouring a kettle etc. painful and often causes sharp spasms when it gets ‘stuck’.
Aside from offering injections, one can also be offered a subacromial decompression. This involves shaving the underneath of the acromium to allow for smoother movement of the tendon.
Firstly, if that makes sense, i’m not paticularly sensible. If it is an upset tendon that is irritated , why shave the bone to allow it space rather than address the tendon? Why an go through an operation, the most common shoulder operation, along with general anaesthetic?
A recent Cochrane review found very little benefit of a decompression compared with physiotherapy ( or even better, osteopathy!) A survey of UK orthopaedic surgeons (Shoulder and Elbow 2015) found broad agreement that it should not be considered for subacromial impingement witout first trying two steroid injections and three months of conservative treatment.
So, we know about the steroid injections. They can be, and often are, very helpful for the bursitis but in my experience, the mechanical effects of a dry needle are comparative to the chemical effects of wet (steroid) needle. My experience is also that it is more likely to take 3 sessions to help alieve the condition than 3 months.
I recall Prof Eyal Lederman saying that he had ‘tendonitis’ in each shoulder. For one he had the surgery and the other conservative treatment. The result was the same. Although, the one bears scars.
Research and evidence does not support a subacromial decompression, certainly not as a first, second or third step.
Instead, address the muscle and tendon ( together with the whole cuff), address the joint space conservatively and the effects should relieve. Add in some rehabilitation exercises and you should be on your way to a pan-free shoulder.